ONLY ONE VESSEL IN UNSTABLE ANGINA OR
ACUTE MI
In a Western European hospital a young patient had PTCA for
angina. He had lesion in two vessels. The presumed culprit lesion
was dilated. Patient had chest discomfort on the table. Operator
thought that the other lesion must be the culprit lesion. He dilated
the other lesion also. A few hours later patient had chest pain
with shock. The angiogram revealed that both vessels have occluded
and patient died in the cath lab
In unstable angina or acute MI there are higher chances of acute
occlusion and other vessel should have been done at least 7-8
hours later..
POOR GUIDING SUPPORT & CHANGING THE
GUIDING CATHETER
In above situation if you are changing the guiding catheter
while the guide wire is across the lesion, it is helpful to leave
a loop of the guide wire in the aortic root to adjust for the
manipulation of bringing in the new guiding catheter.
RCA CLOCK WISE ROTATION
If you are using a judkins guiding catheter into the RCA system
and you are having problem with balloon support that the guiding
catheter is coming back. Just give a gentle clock wise rotation
to the guiding catheter and push very little, it will give a very
stable system in most RCA
LAD ANTI CLOCK WISE ROTATION
If you are having problem like mentioned above in RCA and you
want similar support in LAD then just give a gentle anti clock
wise rotation while giving a very gentle push to the guiding catheter.
MILD CHRONIC RENAL FAILURE & PTCA
In a South Asian hospital a male patient with mild renal dysfunction
underwent PTCA. It was a prolonged procedure requiring extra contrast.
The patient developed anuria but accidently fluids continued causing
pulmonary oedema. With subsequent fall of BP he occluded at the
initial lesion sites. He died during repeat PTCA.
In above situation:
Use a non-ionic contrast
Avoid dehydration, start IV fluids before PTCA and continue
them during and after PTCA.
Some operators use mannitol and frusemide infusion during and
after PTCA
If multi-vessel PTCA then stage the procedure so that contrast
dose of one vessel is washed out before procedure on second vessel
is undertaken thus you will avoid further renal damage.
Above precaution can also be used during diagnostic procedures
in patient with renal failure.
OVER THE WIRE SYSTEM AND
LEFT MAIN DISSECTION
Note - In over the wire system an introducer is not required as
the balloon itself can be used as an introducer and wire is advanced
beyond the balloon while it is lying in the guiding catheter.
In a South Asian hospital an over the wire system
was being used. The operator forgot to advance the guide wire beyond
the tip of balloon. The balloon tip lifted a flap in the left-main
coronary artery and the patient was sent for surgery.
REUSE OF A BALLOON &
LEFT MAIN DISSECTION
In a South Asian hospital a patient underwent PTCA for restenosis
in proximal left anterior descending artery. The lesion was easily
crossed with the wire, then a used balloon was inflated. During
inflation the balloon ruptured at its proximal end and it was withdrawn.
The injection after this revealed that the result at the lesion
site was excellent but a type C flap had developed extending from
near ostium of LAD(site at which proximal end of the balloon was
placed) to the mid left main. The patient was referred for urgent
CABG.
Note - As mentioned earlier if you are reusing
the catheter or the balloon, mark it with an ink to tell you the
number of times it has been used. Do not use a very old balloon
for critical proximal lesions.
AUTO-HAEMOPERFUSION IN PTCA
The technique of Auto-haemoperfusion involves that the syringe which
is used for contrast injection is exchanged for 10 ml. syringe if
the syringe was of larger caliber.
Patient’s own blood is withdrawn in the
syringe and then it is forcibly injected back. During this process
the guiding catheter is kept canulated in the coronary artery. It
gives the advantage of injecting the saturated blood into the coronary
artery. Its useful for the following situations :-
A. After air has been accidentally injected into
the coronary system. The forceful blood injection tends to push
the air emboli out of the coronary vasculature.
In a South Asian hospital large amount of air
was injected in the left system. Above procedure was very helpful.
The cause of trouble was that procedure was long and the small
bottle containing the contrast media was empty and was now supplying
air into the system.
"IF YOU HAVE SEEN HAVE SEEN AIR COMING INTO
THE CORONARY FIRST YOU SHOULD SUCK (the guiding catheter) WITH THE
SYRINGE AND MAKE SURE BLOOD IS COMING BACK, BEFORE REINJECTING BLOOD
AS THERE MAY BE SOME FURTHER AIR BUBBLES IN THE GUIDING CATHETER
FROM WHEREVER THE AIR ENTERED IN THE FIRST PLACE."
B. CLOT IN THE CORONARY ARTERY.
If you visualize a clot into the coronary artery
which was not noticed before then by autohemoperfusion you can push
it towards the distal system and then handle the clot in the distal
coronary vasculature. This has the advantage that
Less myocardium will be at risk in distal vasculature.
If the clot is in proximal LAD then during the
procedure it will not accidentally get pulled back and come into
the left main or go into the proximal circumflex.
C. CLOT BUILDING IN THE LEFT MAIN CORONARY ARTERY
There is occasionally the odd but fortunately
very rare situation during angioplasty that a clot develops somewhere
in the left-main. It can a be a very dangerous situation if the
clot increases in size and attracts more platelets and other clotting
factors. This will put the patients life at risk. It is better to
resort to autohaemoperfusion. So that this clot is pushed somewhere
into the distal bed where once again it will be easier to handle
it.
Such an event happened in a South Asian hospital
and only with hindsight the operator realised that autohaemoperfusion
would have been very useful.
D. POOR MAN’S INTRA-AORTIC BALLOON
An intraortic balloon is a very useful device
to maintain the circulation in the situation of a circulation collapse.
Should you not have access to the balloon, injecting patients own
blood, which is drawn from arterial circulation and pushing it into
the coronary circulation will help in perfusing the myocardium while
you have this difficult situation. Since the catheter (guiding or
diagnostic) is lying in the same vessel, it will be perfusing the
myocardium in the territory whose blood supply has been jeopardized
and causing the patient to have this problem.
NOTE -You cannot try this technique if the patient has developed
the problem and the guiding catheter or the diagnostic catheter
is wedging into the system and is not showing pressure in that situation.
In such an event you have to remove the catheter and not attempt
autohaemoperfusion. Always try to use a leur-lock syringe
during angioplasty.
CLOT IN TOTAL OCCLUSION
All of us enjoy tackling total occlusion but if it is present for
more than a week. It can involve one major problem that once the
circulation stops a clot forms which its always very difficult to
recognize in diagnostic film. Once we have passed the guide wire
and dilated the artery with balloon then we may have a clot which
has started floating This is a very major problem if the vessel
concerned is proximal LAD.
In a South Asian hospital after dilating a proximal
total occlusion a lot was pulled pack with the balloon into the
left-main. Operator ditaled the balloon again in the proximal
left main and then slowly pushed the guiding catheter (size #7 French)
up to the proximal LAD (up to the guiding catheter slightly on the
balloon and withdrew the whole assembly and fortunately the clot
was pulled back.
In another event after dilating a lesion such
as above a clot was pulled and it went in a circumflex artery.
With the balloon the clot was pushed up to the distal Cx. It did
not dissolve with the Urokinase and balloon angioplasty had to be
done at this site(there was no lesion here perior to PTCA and a
substrate for restenosis was created).
So if you are tackling a total occlusion in proximal
LAD and you have deflated the balloon after adequate inflation,
then do not pull the balloon back but instead push it over the guide
wire towards the mid/distal LAD. Wait there then bring the balloon
back towards the lesion and while maintaining the negative pressure
push it again into the mid/distal LAD. After doing this maneuver
2 or 3 times pull the balloon back into the guiding catheter.
This pushing of balloon 2 or 3 times in mid/distal
LAD will hopefully push any clot which may be there towards the
distal bed and not bring it back towards the left main, or transfer
it into the proximal circumflex.
NOTE - Maintain decent negative pressure so that
the profile of balloon is less and it is not rubbing badly against
the endothelium and an injuring it, as the distal vessel gets smaller.
BALLOON PROFILING
One of the major problem in angioplasty is the cost of consumable
items. To cut the cost of consumables, we try to reuse them in several
centers across the world to reduce the overall cost of angioplasty.
One problem in reuse of the balloon is that the balloon profile
is increased and the balloon becomes difficult to handle. To reduce
the balloon profile, take one of the guide wire staightners which
has a decent lumen. Now put the stiff end of the guide wire through
the staightner and push the balloon into the staightner. When balloon
is lying in the staightner ask you colleague to inflate the balloon
to one or two atmosphere and then deflate it to negative pressure.
This will attach balloon to the inner plastic of staightner, Now
gently rotate it clockwise or anti-clockwise whichever movement
you enjoy, and continue maintaining the same movement, i.e. clockwise
or anti-clockwise, untill you find that the movement of the staightner
is totally free over the balloon. This way the balloon will be wrapped
over on the guide wire and the balloon profile will be reduced.
Now you can pull the guide wire out of the balloon and use the balloon
which now has a very low profile.
NOTE - Whatever movement you use, initially the clockwise or anti-clockwise,
please continue with the same rotation and do not change the direction
of rotation.
DEPLOYED STENT COMING BACK
IN THE LEFT MAIN
In a South Asian hospital a one half of deployed stent ( the
stent had two halves which are not joined together) came back in
left main.
The artery planned was proximal LAD. After inflating
the balloon and when we brought the balloon back, the proximal half
of stent came back and got lodged in the left main. The stent was
deployed. It would be very difficult to extract the stent out of
the left main and putting snares or other devices and handling them
into the left main would have invited a great risk. The dilated
lesion in LAD was showing good result. If we sent this patient to
the operating room, then only indication for patient to go for heart
surgery would have been to remove this deployed half stent from
the left main. Since the patient was totally stable, few of us gathered,
debated and decided to fully deploy the stent into the left main
and closely observe the patient for the next six months (left main
restenosis). The decision to reinflate the stent in left main was
taken because the left main was 3.5 millimeter but the stent was
only 3 millimeter. We had taken a balloon which was chubby, an old
balloon and of a high profile We had selected the chubby because
of its length (9mm) as the half stent was only eight millimeter
in length. The guide wire was passed extra and it was making a curve.
Fortunately balloon caught some where in stent and the stent started
moving with the balloon. Author held his breath and gently continued
with the same movement and found that the proximal half of the stent
had moved with the balloon and got imbedded into the distal half
of the stent. Author reinflated the proximal half with the 3.5 millimeter
chubby into the proximal LAD. On his way back that day author went
to the temple first before going home as it was only luck not skill
for above success.
This patient incidentally developed restenosis
which did not involve this proximal half of the stent or left main
and involved the distal half of the stent which was not reinflated
with the chubby balloon. It was inflated only with the initial dilation
with the same balloon on which the stent was mounted.
With the hindsight author tried to assess what
was the reason that the stent was pushed back into the LAD and realize
that there may be 2 factors.
a) The next balloon being used was old so it had
very high profile and a high profile balloon is quite likely to
catch into some facet of stent.
b) Operator had pushed the guide wire more and
guide wire was going obliquely across the stent and was making a
curve. The curve of guide wire into the stent will make it more
likely for the balloon to catch into the facet of the stent and
the stent moved with the the balloon.
Please note that the stent was Micro stent. The
wire edges are fused proximally and distally. If it was something
like bare stent which has free hanging edges at the 2 ends of the
stent. It will make it difficult for balloon to move forward.
Lessons from the case
A Do not use stents which have free parts.
B If such event occurs push guide wire an extra
length and use a high profile balloon or alternatively release negative
pressure when balloon is in stent.
BARE STENT AND BALLOON RUPTURE
Mounting a bare stent on a balloon has been
complicated by rupture of balloon by many operators. They often
blame it on using an old balloon. When you are loading a bare J&J
on a new balloon or old, please do not rotate the bare stent over
the balloon while crimping it because the J&J stent has free
hanging edges at both ends. This rotation will invite some edges
to get imbedded into the balloon during crimping. It will rupture
at that site during inflation where it had embedded, so please do
not rotate the stent while you are crimping it over the balloon.
LOADING HALF BARE
STENT
If you have cut a bare stent into the two halves
and loading it on a balloon. Please make sure that the cut edge
is facing the distal end of the balloon and on the proximal end
of balloon the edges are as the manufactures have supplied. The
reason being that when we cut it with the scissors that point its
likely to be sharp, and if it is facing the proximal end, it is
likely to get caught into the endothelium and injure it, whereas
if it is facing the distal end of the balloon it should smoothly
shift into the vessel.
STENT VISUALIZATION
Some stents have a main problem that they are
not visible on the X-ray machine. Although we find that on a modern
digital machine they are faintly visible. Before deploying the stent,
sprinkle it with some undiluted contrast media while it is on the
balloon, and wait for a few minutes to let it dry slightly. This
will render your stent more visible on your X-ray equipment for
about 5 to 10 minutes, before the contrast is washed away by the
blood stream. Please note that ionic contrast also prevents the
clot formation.
WIRE IN FALSE LUMEN
If during an angioplasty the wire has gone in a false passage
then leave this wire in the false passage and take a new wire.
Now manipulate the new wire. This wire is likely to go into the
true lumen as the previous wire is blocking the entry into the
false passage. You may then remove the first wire from the false
passage.
OCCLUSION OF THE ARTERY DURING GUIDE WIRE
MANIPULATION
If the vessel has occluded during the guide wire insertion,
a floppy wire is more likely to go in the true lumen.
PRIMARY PTCA AND OVER THE WIRE SYSTEM
If you do a Primary PTCA always use an over the wire system
as we do not know the anatomy well and it may require several
changes of balloon or the wire.
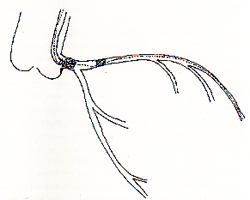
UNCOILING OF A STENT AND PROXIMAL END
COMING INTO THE GUIDING CATHETER
In a South Asian hospital a patient had a coil stent implanted
in the LAD. He developed restenosis and underwent second angioplasty.
Balloon was inflated in the stent (high pressure inflation). When
the balloon was being pulled back, the proximal end of the balloon
got caught in the stent. It uncoiled (proximal part) and was pulled
with the balloon. The metallic wire (uncoiled stent) was pulled
across the left main into the guiding catheter. The operator tried
to hold it with a snare but the wire (uncoiled proximal part of
stent) came out of the guiding catheter into the aortic root.
It took a very long time to catch the wire in the aortic root
and remove it with a snare. When pulled entire stent uncoiled
and came out. The patient had successful angioplasty using a high
torque floppy wire and a second stent was implanted.
With hindsight operator and others thought that if initially when
the wire(uncoiled proximal part of stent) was in guiding catheter,
if a short balloon was used and inflated catching and compressing
the wire in guiding catheter, the entire assembly could have been
easily taken out.
Note - After the initial PTCA the proximal part of the stent
was in the left main at the circumflex ostium. The flow in the
circumflex artery would not have allowed epithelialisation of
the proximal part of stent and it got caught in the balloon. Therefore
when deploying a stent in proximal LAD or proximal Cx make sure
that it is out of left main before deploying it and LAO caudal
view is very useful for this.
Avoid using a coil stent as they also develop concertina effect,
but the GR-II stent has a shaft and is likely to be free from
above problems
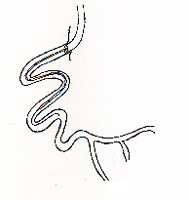
TORTUOUS ARTERY BEFORE THE LESION
In the above situation only a balloon should be used, and only
an over the wire balloon system with a high torque floppy wire
should be used. While advancing the wire keep advancing the balloon
also to tackle the curves while giving support to wire.
STENT AT AN ANGLE
In a South Asian hospital an operator was deploying a stent
with two halves joined together at one point. The stent joint
was placed at the angle. After deploying the stent, the arterial
wall tissue prolapsed in the joint as it separated. With repeat
inflations the problem only got worse. Finally a half stent
was deployed at the site.
In such situations avoid joint at angle. and keep the shaft
of the stent at the angle.
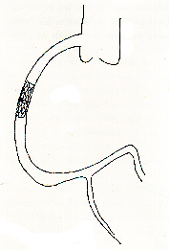
SHORT BALLOON
In a South Asian hospital a patient with a lesion at distal
RCA where it was dividing into four branches. Using the standard
balloon, with center at the lesion, will tear the branch due to
distal balloon. If the balloon was kept proximal then the contents
will spill in distal RCA. A short balloon (High Energy) was used
to avoid above complications with excellent success. There was
no clinical restenosis at 12 month follow-up.

ACUTE OCCLUSION AND PERFUSION BALLOON
CASE A
In a Western European hospital a 36 year old lady underwent
Directional Coronary Atherectomy (DCA) to mid RCA. It was a 3.5mm
vessel. Six hour later she had occlusion of the artery (time mid-night).
She was transferred to Cath-lab immediately. A repeat PTCA was
done using a high torque floppy wire and standard balloon. Good
flow was established but artery occluded again within minutes.
She underwent repeat PTCA with same hardware and intra-coronary
thrombolytic (TPA) was given twice. She had started bleeding profusely
form groin site (11F DCA sheath). PTCA with above hardware was
done several times with groin pressure and continuous blood transfusion
(profuse bleeding). When several above attempts failed and this
combination of profuse groin bleeding and RCA occlusion continued
Operator decided to use a perfusion balloon, which was inflated
at 2 atmosphere for 30 minutes. There was no reocclusion after
this inflation. A six month follow-up angiogram revealed good
LV function and no restenosis.
CASE B
In a South Asian hospital a patient had acute occlusion in mid
circumflex after PTCA with balloon only. Operator implanted a
stent but the artery reoccluded. Intra-arterial Urokinase was
given but again occlusion developed. A reperfusion balloon was
inflated for nearly 20 minutes. This was not followed by reocclusion.
In acute occlusion there is role of arterial wall injury. Prolonged
inflation with a perfusion balloon, is likely to smoothen out
the wall and reduce chances of reocclusion.
LIMA-LAD GRAFT AND NATIVE LAD PTCA
The LIMA-LAD graft is the most popular graft. This graft occasionally
faces problem at the anastomotic site.
In a South Asian hospital a patient had severe anastomotic stenosis.
Native artery had a lesion in the proximal LAD. Patient underwent
PTCA for native LAD.
Note - the LIMA will provide an excellent support during the
procedure and also if patient developed restenosis. This step
was considered safer than handling the anastomotic site.
REMOVING A FOREIGN BODY
Use a device you are happy with.
A biplane system is very useful. If your lab is not equipped
with a biplane system, ask the radiographer to bring the mobile
image intensifier (available in most hospital) and use it in conjunction
with the cath-lab as it will provide a biplane imaging system.
PTCA OF AN ABERRANT ARTERY
In a South Asian hospital a patient was posted for PTCA of a
proximal segment of an aberrant circumflex. During placement of
a guiding catheter a dissection developed at the ostium and the
artery was occluded.
Note - if placement of a guiding catheter is difficult then
use a 6 or 7 French guide to avoid complication as above.
REMOVING A KNOTTED SWAN
In a Western European hospital a swan ganz catheter had knotted
in the right-atrium. It was inserted via the right subclavian.
In cath lab the knot persisted despite a long trial. Then a
snare device was inserted via the right femoral vein. It caught
the proximal part of catheter in right atrium, then swan ganz
catheter was pulled with tension thus the knot became tight and
smaller in volume. The catheter was cut near the subclavian entry
site and rest of the system was pulled out from the femoral vein.
The tear in the vein could be controlled by gentle prolonged pressure.
Note - It is easy to control the tear of vein at the femoral
site than the subclavian or jugular.
PRESSURE FROM COMPANY REPRESENTATIVES
In a Asia-pacific hospital a company representative was present
in cath lab. The operator decided to go for his stent. He was
not very familiar with this unit and the patient developed a major
dissection and was sent to surgery.
Note - Do not allow the company representatives to physically
frequent your cath lab as it can put unwanted pressure in choosing
a hardware.
DISSECTION OF THE ARTERY WITH THE GUIDING
CATHER
In a south Asian hospital a DCA of a severely stenosed RCA was
planned. When the operator was introducing the DVI guiding catheter,
it went deep into the artery and dissected the proximal segment
of the artery. After this dissection the artery was totally occluded.
This artery could not be salvaged. It was a infarct related artery
and had retrograde filling from the normal left system. The operator
decided not to refer this patient for surgery.
Note Always be careful with a large size catheters.
DO NOT ALLOW THE PATIENT TO PUSH
YOU FOR A PRODEDURE
In a Asia Pacific hospital a patient had a totally
occluded dominant RCA. The LAD was supplying collaterals to it and
it was diseased proximally. The operator could not open the RCA
and wanted to refer the patient for CABG but the patient pushed
him into the PTCA of LAD. During the implantation of the stent the
patient had a cardiac arrest and could not be revived.
Note - Do not be pushed by patient’s desire
and work against your conscience.
BE GENLE WITH THE GUIDE WIRE
In a South Asian hospital the patient was undergoing
PTCA for a proximal LAD lesion.. The operator was rough with the
guide wire and the LAD was totally occluded and patient had to be
referred for CABG.
BIFURCATION STENTS
In an Asia Pacific hospital a patient underwent
PTCA and stent for a bifurcation dominant Cx and OOM lesion. The
patient had a cardiac arrest same night and died in CCU.
If you want to implant a bifurcation stent think
twice.
If the branch is not big do not plan such a procedure.
If you committed for such a procedure then first
place a stent in the main vessel and leave it undeployed. In branch
deploy a stent(radio-opaque) with round edges. Now pull the assembly
from the branch and deploy the stent in main artery.
Some operators prefer to debulk such lesion with
DCA.
PDA MEASUREMENTS
In a South Asian hospital PDA was undersized and
soon after the deployment the coils embolized. They could be removed
with snares but with lot of difficulty.
LARGE PDA
In a South Asian hospital an operator planned to
use an ASD device in a large PDA. The child died during the procedure.
Do not be adventurous as it is the patient’s
life which is at risk.
LA RUPTURE IN PTMC
In a Western European hospital a patient was taken
for PTMC. The innoue balloon was giving difficulty in being negotiated
into the LV. During this the patient became hypotensive and had
to referred for urgent surgery. The surgeons found a small tear
in LA. The operator could not figure out that how it happened.
STENT RETRIEVAL
Most stents are visible undeployed.
If the stent has not come off the balloon inflate
the balloon to 0.5 or 1 atmosphere and try to pull back.
It has come off the balloon and the balloon is
pulled back.
Pass few wires beyond the stent and entangle
the distal end of the wires and pull them simultaneously.
If above fails pass a wire by the stent and crush
it in the vessel wall.
|